Periodontal
Topics on this page
Periodontal Treatment
If you've been diagnosed with gum disease, there are a variety of treatment options depending on the details of your situation and the severity of the problem. We always start with the least invasive options, which are non-surgical. However, in more advanced cases, surgery may be necessary.
Gum Disease
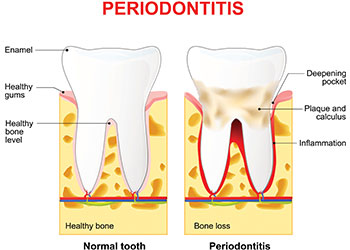 Gum disease is caused by a buildup of plaque (a sticky form of bacteria that forms on the teeth). If the plaque is not removed (by flossing, brushing, and regular dental checkups), it will continue to build up and create toxins that can damage the gums. Periodontal disease forms just below the gum line and creates small pockets that separate the gums from the teeth. Periodontal disease has two stages: gingivitis and periodontitis. Unless the disease is treated, it can ultimately lead to tooth loss.
Gum disease is caused by a buildup of plaque (a sticky form of bacteria that forms on the teeth). If the plaque is not removed (by flossing, brushing, and regular dental checkups), it will continue to build up and create toxins that can damage the gums. Periodontal disease forms just below the gum line and creates small pockets that separate the gums from the teeth. Periodontal disease has two stages: gingivitis and periodontitis. Unless the disease is treated, it can ultimately lead to tooth loss.
Non-Surgical Treatment
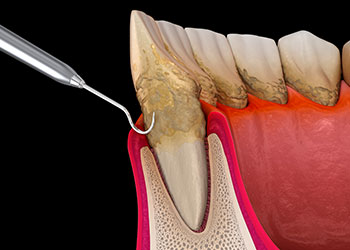 The first line of defense against gum disease is a unique type of cleaning called “scaling and root planing.” In this procedure, an ultrasonic cleaning device is used to remove plaque and tartar from your teeth where regular cleaning devices can't reach: under the gum line, on the tooth, and around the root. Then, the rough surface of the tooth and the root are smoothed out (planed). This provides a healthy, clean surface that makes it easier for the gum tissue to reattach to the tooth.
The first line of defense against gum disease is a unique type of cleaning called “scaling and root planing.” In this procedure, an ultrasonic cleaning device is used to remove plaque and tartar from your teeth where regular cleaning devices can't reach: under the gum line, on the tooth, and around the root. Then, the rough surface of the tooth and the root are smoothed out (planed). This provides a healthy, clean surface that makes it easier for the gum tissue to reattach to the tooth.
If you address your gum disease before it becomes severe, scaling and root planing may be the only treatment you need. However, as with any dental procedure, after-care is vital. In order to keep your teeth in good shape and resist future occurrences of gum disease, you must brush and floss daily, eat a healthy diet, avoid tobacco use, and have regular dental checkups. Even after a successful scaling and root planing, if you don't attend to your teeth properly, it's quite likely that you'll develop gum disease again.
Surgical Treatment Options
If the tissue or bone surrounding your teeth is too damaged to be repaired with non-surgical treatment, several surgical procedures are available to prevent severe damage and to restore a healthy smile. We will recommend the procedure that is best suited to the condition of your teeth and gums. Following is a list of common types of periodontal surgery:
-
Pocket Depth Reduction
In a healthy mouth, the teeth are firmly surrounded by gum tissue and securely supported by the bones of the jaw. Periodontal disease damages these tissues and bones, leaving open spaces around the teeth that we call pockets. The larger these pockets are, the easier it is for bacteria to collect inside them, leading to more and more damage over time. Eventually the supportive structure degrades to the point that the tooth either falls out or needs to be removed.During pocket reduction procedures (also known as “flap surgery”), we fold back the gum tissue and remove the bacteria hiding underneath, as well as the hardened plaque and tartar that have collected. We may also remove any tissue that is too damaged to survive. We then sew the healthy tissue back into place. Now that the tooth and root are free of bacteria, plaque, and tartar, and the pockets have been reduced, the gums can reattach to the teeth.
-
Regeneration
When the bone and tissue supporting the teeth have been lost due to severe gum disease, we can restore these areas with a regeneration procedure. During this process, we begin by folding back the gum tissue and removing the bacteria, plaque, and tartar. Depending on your situation, we may then perform a bone graft to stimulate new bone growth, or we may apply a special kind of protein that stimulates tissue growth to repair the areas that have been destroyed by the disease.
Soft Tissue Grafts
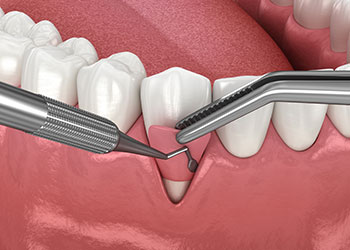 Your gums may have receded for a variety of reasons, including aggressive tooth brushing or periodontal disease. You may not be in control of what caused the recession, but prior to treatment, your periodontist can help you identify the factors contributing to the problem. Gum grafting will cover the exposed roots to protect them from decay, help reduce tooth sensitivity, and improve the aesthetics of your smile. Whether you have a gum graft to improve function or aesthetics, you'll probably receive the benefits of a beautiful new smile and improved periodontal health - your keys to smiling, eating, and speaking with comfort and confidence.
Your gums may have receded for a variety of reasons, including aggressive tooth brushing or periodontal disease. You may not be in control of what caused the recession, but prior to treatment, your periodontist can help you identify the factors contributing to the problem. Gum grafting will cover the exposed roots to protect them from decay, help reduce tooth sensitivity, and improve the aesthetics of your smile. Whether you have a gum graft to improve function or aesthetics, you'll probably receive the benefits of a beautiful new smile and improved periodontal health - your keys to smiling, eating, and speaking with comfort and confidence.
Gum Recession
Gum recession is caused by advanced gum disease. When gingivitis goes untreated, gum disease (also called periodontitis) will cause gums to pull away from the teeth, leaving deep pockets where bacteria can grow and damage the bone that supports the teeth. Gums can also shrink back from the teeth, making the teeth look longer. Teeth may then become loose, fall out, or have to be pulled out by a dentist.
Do you have gum recession?
Gum recession does not happen overnight. You may not even notice that your gums have receded, as it is a very slow, gradual process. However, without a gum tissue graft, recession can have a detrimental effect on the health and function of your teeth. If your dentist has diagnosed you with gingivitis or periodontal disease, it is important to notice if:
- You have sensitivity to hot or cold temperatures, or even to sweet, spicy, or sour foods
- Your teeth appear longer than normal
- Spaces between your teeth seem to grow
- The roots of your teeth begin to show
Gum Tissue Grafting
When you come to our office for your grafting procedure, a local anesthetic will be given to numb the areas involved. You may also receive medicine to help you relax. We want your experience in our office to be as comfortable as possible, so let us know if there is anything you need during your procedure.
Depending on your specific needs, your periodontist will perform one of three different types of gum tissue grafts.
- Connective tissue grafts: The most common method to treat root exposure, connective tissue grafting involves your periodontist cutting a flap of skin on the roof of your mouth (or palate) and removing tissue from under the flap, called sub-epithelial connective tissue. This tissue is then stitched to the gum tissue surrounding the exposed root. After the connective tissue, or graft, has been removed from under the flap, the flap is then stitched back down.
- Free gingival grafts: Similar to a connective tissue grafting, a free gingival graft involves the use of tissue from the roof of the mouth. But instead of making a flap and removing tissue under the top layer of flesh, a small amount of tissue is removed directly from the roof of the mouth and then attached to the gum area being treated. This method is used most often in people who have thin gums to begin with and need additional tissue to enlarge the gums.
- Pedicle grafts: In this procedure, instead of taking tissue from the palate, it is grafted from gum around or near the tooth needing repair. The flap, called a pedicle, is only partially cut away so that one edge remains attached. The gum is then pulled over or down to cover the exposed root and sewn into place. This procedure can only be done if you have plenty of gum tissue near the tooth.
Many factors will contribute to your chosen grafting technique. Your periodontist can tell you which method will work best for you, your health, and your smile.
Bone Grafts
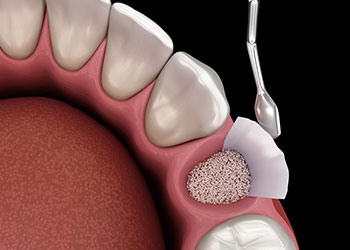 Also called regenerative surgery, a bone graft is used to recreate bone and soft supporting tissues lost due to periodontitis. If you have periodontitis, you may be losing bone support around your teeth, and in order to avoid extractions, your periodontist may recommend regrowing the lost bone with a graft.
Also called regenerative surgery, a bone graft is used to recreate bone and soft supporting tissues lost due to periodontitis. If you have periodontitis, you may be losing bone support around your teeth, and in order to avoid extractions, your periodontist may recommend regrowing the lost bone with a graft.
The goal of bone grafting is to encourage the body to rebuild the bone and other structures that attach a tooth to the jaw. First, your periodontist will separate the gums from your teeth in order to gain access to the roots and bone. The roots will be thoroughly cleaned, and the holes in the bone will be filled with a graft material that usually consists of your own bone. After this process is completed, your periodontist will put the gums back in place and stitch them together. Over the next few months, the grafted material will be encouraged to grow, which will fill in for lost bone and soft tissue.
Bone Regeneration
If you are experiencing gum disease and your periodontist has noticed a loss of bone as well, bone regeneration may be a good option to restore the health and function of your smile. Bone regeneration is a periodontal surgical procedure that regenerates jaw bone and tissue in order to correct the damage caused by periodontal disease. Bone regeneration is often performed to protect your existing teeth and the soft tissues that keep them in place so that you can experience an enhanced quality of life as a direct result of improved health, function, and appearance.
Bone regeneration can also benefit patients with missing teeth and those who don't qualify for dental implants. Dental implants require a significant amount of jawbone prior to the procedure in order to be successful. Bone regeneration can help patients who suffer from a deteriorated jawbone support their restorations or prepare for an implant dentistry procedure.
The Bone Regeneration Procedure
During this procedure, your periodontist will place a biocompatible membrane between the gum and bone, which acts as a barrier. This barrier prevents down growth of the gum into the underlying bone as it heals. In some cases, a bone graft or tissue-stimulating proteins may be placed under the membrane to encourage your body's natural ability to regenerate bone and tissue. Membranes around teeth are typically designed to dissolve away or reabsorb after a few weeks. There are many options to enhance support for your teeth and to restore your bones to a healthy level.
Crown Lengthening
If you feel your smile is "gummy" or if you think your teeth are too small, crown lengthening may be right for you. Crown lengthening is a procedure performed by your periodontist to reshape the gum line to improve the aesthetics of your smile by exposing more of your teeth.
Crown lengthening involves removing excess gum tissue around the upper teeth to make them look longer. If the gum line is uneven, crown lengthening can also sculpt the gum line to produce a more symmetrical, balanced smile. Crown lengthening may be done for dental care and medical reasons as well as for cosmetic purposes. If your periodontist finds decay or fracture under the gum line, for example, crown lengthening can help expose more of the tooth's crown in order to support a filling or restoration.
Crown lengthening is done under local anesthesia, so as the numbing effect wears off, you may feel some discomfort along your new gum line. You will most likely be prescribed pain medication, so it is important to let us know what other medications you are already taking. Usually, a follow-up appointment will be needed to check the healing process and remove any stitches.
Oral Pathology
Our office is not only dedicated to your smile, we're also dedicated to your overall wellness. We take a holistic approach to your dental care, which includes an oral cancer screening as a part of your regular exam. Like many kinds of cancer, oral cancer can be life-threatening if not diagnosed and treated early.
We have the skills and tools to ensure that early signs and symptoms of oral cancer and pre-cancerous conditions are identified. While these symptoms may be caused by other, less serious problems, it is very important to visit our office to rule out the possibility of oral cancer. The most common symptoms of oral cancer include:
- Red or white spots or sores anywhere in the oral cavity
- A sore that bleeds easily or does not heal
- A lump, thickening, or rough spot
- Pain, tenderness, or numbness anywhere in the mouth or on the lips
- Difficulty chewing, swallowing, speaking, or moving the jaw or tongue
Our team is trained in a simple, quick screening that involves an examination of your oral cavity as a whole, and not just your teeth, to detect cancerous and precancerous conditions. Besides a visual examination of your mouth, we will also feel the tissue of your mouth and throat to detect any abnormalities. If we find an area of concern, we may perform a simple test, such as a brush test, which collects cells from a suspicious lesion in the mouth to be sent to a laboratory for analysis. If this test comes back atypical or positive, we may recommend a biopsy.
Hygiene & Maintenence
Scaling and root planing is one of the most effective, non-surgical ways to treat gum disease before it becomes severe. Scaling and root planing clean between the gums and the teeth down to the roots.
Scaling is basically the process of removing dental tartar from the surfaces of the teeth. Root planing is the process of smoothing out the root surfaces and removing any infected tooth structure. If you have gum disease or gum pocketing, the gum pockets around the teeth will have deepened, thereby allowing tartar deposits to form under the gum line. A careful cleaning of the root surfaces to remove plaque and calculus (tartar) from deep periodontal pockets and smoothing the tooth root to remove bacterial toxins will help ensure that your gum disease is controlled.
Helpful Hints to Keep in Mind
- Scaling and root planing does not usually cause much discomfort, but you might experience some soreness afterwards, since deeper regions under the gums have been cleaned.
- Your teeth themselves may become a bit more sensitive to temperature, and bleeding might occur for a little while after your procedure.
- Over-the-counter painkillers, such as ibuprofen, work very well to alleviate discomfort, as do ice packs applied to the outside of the face around the treated area.
- Brushing and flossing will have to be done more gently to avoid aggravating any bruised or tender gum areas. We'll show you the best methods for keeping your teeth clean during this time.